The buzz around the NBA world lately has been around some sad news. If you’ve been following the NBA finals, then you too would know about Kevin Durant’s story. Arguably the best basketball player in the world went out of Game 5, two nights ago, with one of the scariest athletic injuries: the Achilles injury.
If you don’t know what happened, then check it out at https://twitter.com/ProFootballDoc/status/1138277876539650049
The link above will show you a specific video of Kevin Durant tearing his Achilles tendon mid game. Orthopedic surgeon, Dr. David Chao, will even go on to say that he believes it is a complete Achilles tendon rupture. (Source: https://www.sandiegouniontribune.com/sports/nba/story/2019-06-11/nba-finals-kevin-durant-achilles-injury-warriors-free-agency)
While official word from the NBA, i.e. MRI results, have yet to be released, we already know that this injury is bad, bad news as is.
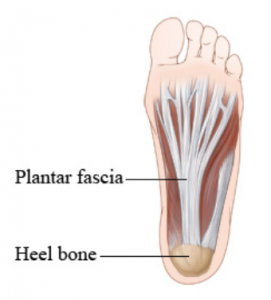
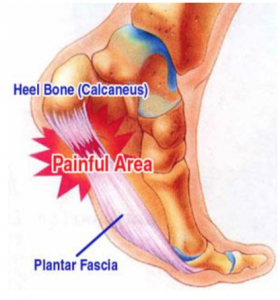
The Achilles tendon is the largest tendon in your body. It connects the large muscles (gastrocnemius and soleus) in your calf to your heel bone (calcaneus). You greatly need it for all the basics of sports activities such as running and jumping. Heck, you need it for just walking!
The Achilles tendon injury is usually the event of a tear in the tendon around 4 to 6 cm above the heel. In some cases, it can happen closer to the heel with such a force that it breaks off a part of the calcaneus.
This injury typically happens in the patient population age 30 to 50 and is sports related. It happens often to a special group of people dubbed, “Weekend Warriors”. Think adults who like to pick up sports on the weekends.
Should you think that you have experienced an Achilles injury like Kevin Durant’s, then ice and elevate your leg. We recommend that you schedule an appointment with your doctor as soon as possible. Your doctor will check for many things such as:
- Swelling and discoloration in the area
- Tendon gap
- Tender and pain
A clinical examination called, “The Thompson Test” will be performed to test the remaining strength and function of your Achilles tendon.
Treatment for this injury can go in either direction between non-operative and operative. Non-operative treatment will require immobilization of the leg, typically by a cast, then rehabilitation. Operative treatment means that the Achilles tendon will be surgically exposed and repaired via suturing. Operative treatment also undergoes an immobilization period and then physical therapy.
Operative treatment is usually recommended for patients who are athletically active. This will most likely be Kevin Durant’s route. Recovery from an Achilles tear can range from anywhere between 4 months to a year. Needless to say, it is a serious injury that requires great attention.
We wish Kevin Durant the best of luck in this process. If you or someone you know may have suffered an Achilles injury, then please give us a call at 1-310-652-3668 to schedule an appointment immediately.


 While most peo
While most peo
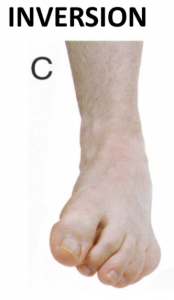
 The most typical incident of an ankle sprain happens when you roll your ankle inward. Although this injury is categorized as the most common athletic injury of all time, it can happen to any ambulatory person of any background.
The most typical incident of an ankle sprain happens when you roll your ankle inward. Although this injury is categorized as the most common athletic injury of all time, it can happen to any ambulatory person of any background.